If you’re a man hooking up with other men, there’s very little you can do to prevent becoming infected with monkeypox.
That’s according to Dr. David Herman, Director of Primary Care Medicine at the Los Angeles LGBT Center, and other experts who participated in the center’s virtual town hall on Tuesday night to address the looming threat of monkeypox, a highly contagious but poorly understood virus that is spreading silently among gay men and trans women in the L.A. area and throughout the world.
The center took questions from patients and the public, bringing together Herman and other doctors to provide answers and clarity on the mysterious disease.
“To be honest about it, it’s spreading right now through intimate content,” Herman said. “And so the reality of the spread of monkeypox is such that really if you’re engaged in intimate contact, you are at risk. It’s a hard question to answer because I don’t think it’s the answer everyone wants to hear, but certainly that’s really where the spread has occurred.”
“If you use Grindr, for example, as a way of hooking up with partners … the people who are using Grindr like to have a lot of sex,” added Dr. Robert Bolan, Medical Director of Research and Education at the center. “And so you’re more likely to find someone who is also having a lot of partners. And so when you have sex with somebody, you’re not only having sex with that person, but you’re having sex with the last three or four people that they had sex with.”
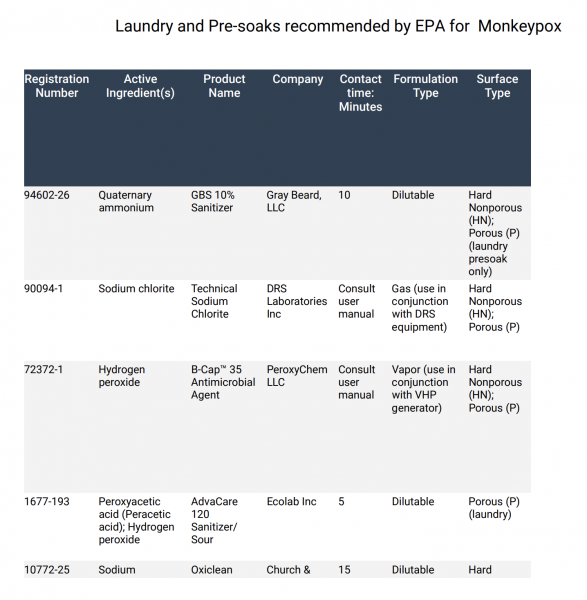
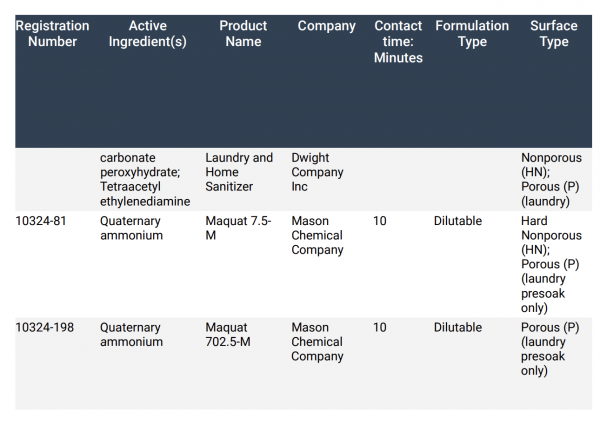
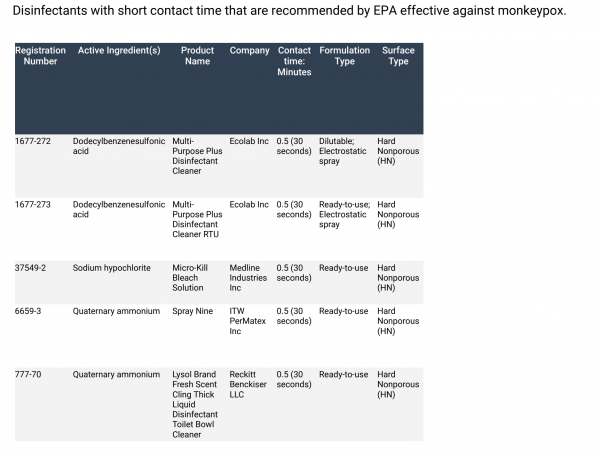
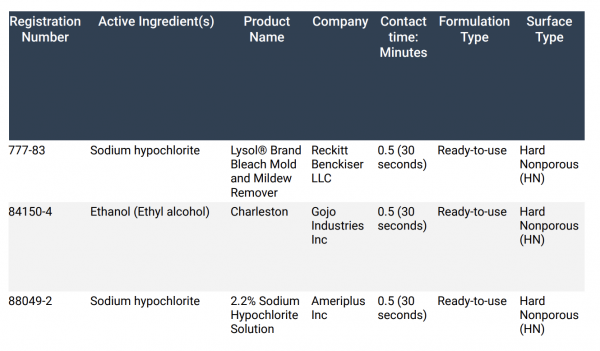
The doctors don’t think condoms will provide much protection from monkeypox — except, perhaps, from a painful internal infection. The virus is very hardy, according to the doctors, and cleaning agents must be left on surfaces longer to kill it. A list of approved chemicals can be found at the bottom of this article.
A monkeypox infection lasting four weeks or longer isn’t unusual. If you get the virus, you remain infectious as long as you have symptoms, and until any scabs have fallen off. Many of the recent U.S. cases have been relatively mild, with many men showing few of the traditional flu-like symptoms, and skin lesions being less widespread and often limited to the genital and anal areas. Experts don’t know whether you can be re-infected with monkeypox or whether a previous infection provides some level of immunity.
How easily transmittable is monkeypox? While it can be spread via large respiratory drops, it more likely requires prolonged close contact – not just casually brushing up against someone. But how prolonged? Three to five minutes of open mouth kissing would qualify, Dr. Bolan said. “It’s got to be some bumping and grinding.”
The monkeypox rash can vary from person to person. It often materializes as redness before the area of skin rises into what’s called a papule, which fills with liquid (becoming a vesicle), then ultimately dries out and falls off.
For the latest information on testing and vaccination, visit https://lgbtnewsnow.org/monkeypox/ or http://publichealth.lacounty.gov/acd/monkeypox/
What is monkeypox?
Monkeypox is a viral infection usually found in animals like squirrels and non-human primates. First identified in humans in 1970, monkeypox has similarities to the smallpox virus but is significantly less severe. Of note, smallpox was eradicated in 1980 as a result of widespread vaccination. Most cases of monkeypox resolve on their own in 2-4 weeks, but approximately 3-6% can die. In the current outbreak, none of the patients have died and the circulating strain appears to be a milder form.
What are the symptoms of monkeypox? How do I know if I have it?
Most cases take anywhere from 7-14 days after infection for symptoms to start. Early symptoms are similar to flu and COVID and include fever, headache, muscle aches, exhaustion and swollen lymph nodes. However, people with monkeypox do not usually have the cough or nasal congestion commonly seen in flu and COVID. These early symptoms may be mild or may not occur at all. Usually within 1-3 days of the flu-like symptoms, patients develop a flat rash that soon progresses to raised bumps, then blisters, then pus-filled bumps. Over the course of two weeks the rash scabs over and resolves. Of note, the rash and other symptoms can look very similar to syphilis, which is far more common in our community.
Because the number of cases of monkeypox in the US is still so low, flu-like symptoms and/or rashes are much more likely to have causes other than monkeypox. However, it is important to be aware of the symptoms of this virus in the rare instance of contact with an infected individual.
What should I do if I have symptoms that are concerning, or think I may have been exposed?
First, it is extremely unlikely that someone without a known exposure will become infected with monkeypox. That said, anyone who develops concerning symptoms of fever and rash should isolate themselves at home or somewhere safe and away from other people and immediately call to speak with their medical provider. Do not walk into the office but call ahead to make sure you can be evaluated and seen without putting others at risk. If you must leave the house to seek urgent medical care, be sure to wear a mask and cover any visible lesions under clothing.
How does monkeypox transmit?
Infection occurs through direct contact with the skin or body fluids of an infected individual, or through prolonged face-to-face contact. This can happen directly through sex and other intimate activities, or indirectly through contaminated items like bed sheets or towels. Unlike COVID, the virus is not airborne and is much more difficult to transmit. It can be transmitted in large respiratory droplets from coughs and sneezes but these generally cannot travel more than a few feet. Casual contact with people in daily life is not known to transmit monkeypox. However, any prolonged physical contact with an infected individual (particularly skin-to-skin contact without clothing) can lead to transmission. There is risk of transmission in all sexual encounters without regard to the gender or sexual orientations of the people involved.
How can I keep myself safe?
The number of cases of monkeypox in the US is extremely low, including in men who have sex with men. To prevent transmission, the same masks, gowns, gloves, frequent handwashing and social distancing that are helping keep us safe from COVID will also protect us from monkeypox. If you have to touch a potentially infected person for some reason, be sure to use proper PPE and dispose of it immediately after contact in appropriate biohazard bags.
Where is this current outbreak?
Monkeypox is usually found in central and west African countries including Cameroon, DRC, Gabon and Nigeria. Since May 18, 2022, over 100 cases have been identified in over 20 countries. What is unusual is most of these cases have no history of travel to the areas of Africa where this virus normally lives. There are now a handful of confirmed cases of monkeypox in the US. As of May 25th, California has one suspected case of monkeypox but confirmation is still pending. Though numbers are still low, the World Health Organization has concerns that there may be many more cases not yet diagnosed.
Are LGBTQ+ people at increased risk for monkeypox?
It is true in Europe that gay and bisexual men make up most of the new monkeypox cases but this is likely a result of coincidental contact with infected people at one or more recent LGBTQ-focused events resulting in a cluster of cases within the community. Good public health should prevent men who have sex with men (MSM) from being singled out as it may result in medical providers missing cases of monkeypox in other populations. It also can lead to further shaming of LGBTQ+ people as our community continues to experience increased stigma related to sexuality and HIV/STIs. The Center will remain a source of judgement-free healthcare for anyone who is showing monkeypox symptoms or any other stigmatized health condition.
Could monkeypox become the new COVID?
This virus is nothing like COVID and has almost no chance of becoming a new global pandemic. Unlike COVID, monkeypox is transmitted only by prolonged physical contact with an infected individual. Casual contact like walking through a supermarket or spending time in a meeting is very unlikely to spread this virus. However, healthcare workers, household members and sexual partners of infected patients are more at risk. Proper use of PPE can drastically reduce this risk even with known cases.
Have there been other outbreaks of monkeypox in the US?
There were 2 travel related cases of monkeypox identified in the US in 2021. These individuals were isolated and there were not any additional infections associated with these individuals. In 2003, there was a larger outbreak in six US states and included forty-seven confirmed cases of monkeypox. As a result of active public health measures, the outbreak was swiftly contained.
What is the Center’s response to this current outbreak?
The Center is closely following the guidance of the CDC and LA County Department of Public Health. Protections put in place during COVID (including masking and physical spacing) are effective in preventing spread of any infectious disease including monkeypox. We will be working with nursing staff and medical providers on ways to distinguish between monkeypox symptoms and those of other infections like syphilis. If one of our patients, clients or staff is suspected to be infected with monkeypox, we will work closely with public health officials to address and contain any outbreak.

Whistling past the graveyard just like during the onset of AIDS.
Boys will be boys.
As of 9am July 15th there were 85 cases in LA County, up from 60 cases on July 11th.(http://publichealth.lacounty.gov/media/monkeypox/)
As of 2pm july 14th there were 250 cases statewide. (https://www.cdph.ca.gov/Programs/CID/DCDC/Pages/Monkeypox.aspx)
Are we going to blame this on Sepi Shyne too? Or is this more of a Lindsey Horvath thing?
Have you guys heard of purple pitcher plant? Google it!
Now if somehow we could have a vaccine against Special Interest Politic Pox on a local level, the city might move forward unaffected and unaffected by the dubious goals of current council members and those aspiring to the task.
Time to get serious folks.
Ever since monkeypox surfaced I’ve been too nervous to even spank the monkey!